In January 2020, Definitive Healthcare CEO, Jason Krantz, hosted his annual healthcare trends webinar:8 Top-Of-Mind Trends for Physician and Hospital Buyers In 2020.
Each year, these trends are developed based on conversations with our 2,500+ clients across the provider, pharmaceutical, biotechnology, medical device, healthcare IT, staffing, insurance, consulting, and financial services industries. The trends are also developed with support from our team of data scientists—who conduct advanced analytics on market trends and disease patterns through our leading data and analytics intelligence software platform.
Did you miss the webinar? Here is a recap, based on our viewers’ interests:
1. Healthcare accelerates its IT journey
Healthcare technology usage is picking up steam, with AI, telehealth, and smart home technologies driving the next wave of innovation. Physician and nursing shortages and a rapidly-aging baby boomer population are creating demand for telehealth options and in-home tech, and augmented intelligence (AI) has been helping radiologists to sift through patient scans faster than ever before.
This type of technology is slated to play more of a supporting role, not a replacement role, in healthcare delivery. With the use of AI solutions, healthcare professionals will see increased efficiencies in their workflow. Any tools that physicians can use to ease staffing shortages, reduce cognitive overload, and improve workflows will be helpful to physicians.
As an example, one of the panelists from our “Value-Based Care in High Cost Physician Specialties” webinar panel, Dr. David Rosman, explained: “AI-driven tech allows me — a radiologist — to see more cases in any given day and work more efficiently than I would otherwise be able to without the use of augmented intelligence technologies.”
2. The tension between data accessibility and data security intensifies
Healthcare wearables, smart home technologies, and even at-home genetic tests are creating enormous piles of data to be synthesized, and everyone wants to get ahold of that information. Patients are requesting greater access to their medical records to help them make informed decisions about their care. Providers want to aggregate disparate patient data in order to use it in a predictive manner. And, unfortunately, the increasing demand for this data is attracting cyber-criminals.
Data breaches, a problem across all different industries, is particularly acute within healthcare. 2019 was the largest year ever for data breaches, with 500 healthcare data breaches affecting over 41 million individual records last year—an increase of 123 data breaches from 2018.
HHS reported healthcare data breaches by year
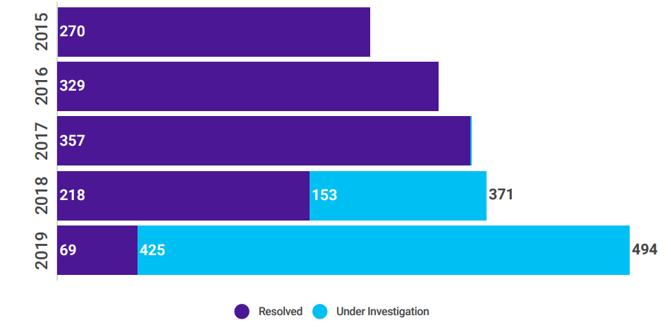
Fig 1: Definitive Healthcare: Healthcare Data Security Year In Review 2019 (Data as of 01/07/2020)
This problem isn’t going away. So how do we manage the balance of accessibility and security? There is a pressing need for proactive approaches to address this data security problem. We recommend:
- Data sharing agreements that set clear expectations of data use that are in line with patient privacy expectations (What is the data? And, how it should be cared for?)
- Employees, contractors, or anyone with data access must have in-depth training on data usage guidelines and understand why these are important. Guidelines should also be regularly updated each year.
- Data access should be restricted. Organizations will need to start thinking about how they cordon off the data on a very need-to-know basis
3. Consumerization 2.0: the patient joins the care team
The classic patient consumer is evolving. Gone are the days of “doctor knows best;” patients now have access to websites like WebMD and are able to arrive at their appointments ready to discuss potential diagnoses, symptoms, and treatments. And now—with the recent boom in at-home genetic testing—patients are better able to understand which conditions they might be at risk for, and how they might prevent condition or disease progression down the road.
The at-home genetic testing market is exploding. At the start of 2019, more than 26 million consumers had added their DNA to four leading commercial ancestry and health databases. While there are still concerns about the accuracy and privacy of these genetic tests, ultimately, the predictive patient could actually decrease overall healthcare costs by (1) changing their behavior and adopting prevention strategies and, (2) detecting health risks and seeking early intervention.
4. Physicians heed the call to become data-driven
Physicians are really starting to embrace data to drive the way they provide care to their patients. As an example, over 73 percent of medical students are currently seeking additional training on innovations in healthcare, according to Stanford Medicine’s 2020 Health Trends Report. They’re trying to stay up to date on what’s happening. Similarly, 80 percent of medical students and practicing physicians are encouraging the use of patient health apps, and another 70 percent of medical students support the use of wearable devices.
Physicians feel that there are real benefits to gather from all of this data collection. With access to more patient health information, physicians can make better, more informed care decisions and potentially lower healthcare costs. But currently, 50 percent of physicians think their patient data access could be improved—with many doctors pointing toward improved access to medication adherence, prescription costs, and clinical history data as top priorities. As technologies continue to evolve and physicians are exposed to new data analytics tools, physician buy-in and interest may increase.
5. Precision medicine increases complexity for physicians
Precision medicine programs in U.S.-based acute care organizations are projected to more-than-double over the next ten years. Demand for these advanced therapies is driven by the personalized healthcare insights provided by wearables and at-home genetic testing kits. But data overload is one of the biggest roadblocks in realizing precision medicine’s full potential.
In the emerging world of precision medicine, new genetic testing products are released at an unprecedented rate and physicians have thousands of different products from which to choose. This presents a problem—as most physicians do not have formal training in genetics or genetic testing and these products often are released before evidence-based guidelines are available to help inform their use. Thus, it becomes difficult for physicians to not only pinpoint which tests to order, but also to interpret the test results and understand the minute differences between results.
6. Providers must contend with wildly different generational care demands
Baby boomers are entering retirement in droves. By 2030, the 65 and older population is expected to outnumber children for the first time in U.S. history—with a projected 1 in every 5 citizens of retirement age. This will signal massive growth in hospice and palliative care markets.
Meanwhile, millennials are driving growth in the outpatient market. This generation is technology and data-driven. They value convenience and cost savings over continuity and are more likely to visit a retail clinic instead of their primary care provider (PCP).
Millennials are also aging into heads of household and increasingly becoming medical care decision makers. This may impact the boomer generation as they elect to enroll their parents in fast, convenient outpatient care and encourage the use of telehealth technologies to keep them out of the doctor’s office.
7. Cost transparency will drive next phase of value-based care
Value-based care (VBC) is not a new concept. Years ago, the Centers for Medicare and Medicaid Services (CMS) implemented incentives and penalty programs to affect lower readmission rates and improved patient satisfaction among hospitals and care providers.
The question is, where does value-based care go from here? Value-based care penalties have significantly impacted revenue streams at U.S. hospitals. According to Definitive Healthcare data, the estimated revenue loss due to readmission penalties has been about $500-600 million per year from 2016 to the present. And, the hospital-acquired condition (HAC) penalty has been similarly large, hovering around $300 million per year.
Revenue loss: value-based care readmission & HAC penalties 2016-2020
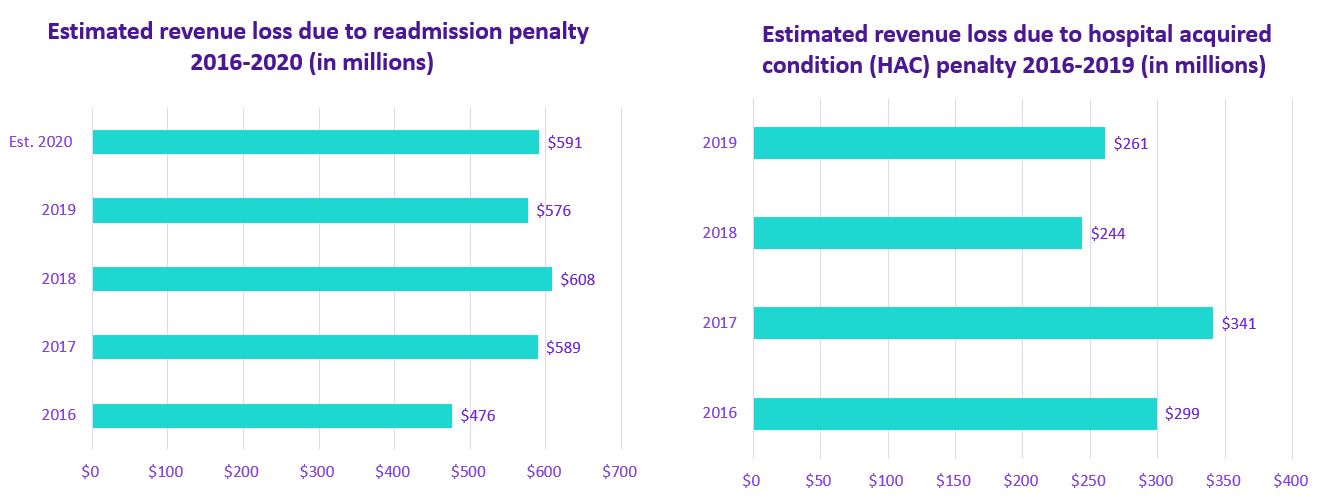
Fig 2: Financial data is from Definitive Healthcare’s Hospitals & IDNs database, accessed January 2020
The good news is that we’ve seen some real benefits from this: readmission rates have declined and the zero-tolerance HAC penalties are starting to enact change in hospitals as well. Going forward, quality will be an important factor in how we make healthcare decisions.
Now, federal price transparency initiatives are changing the future of value-based care delivery models. Patients want to understand the price tags associated with their treatments, employers are trying to figure out how they can bring down their cost of living fees, and physicians want to understand how they can provide high-quality care at a lower price point—particularly as they start to take on more risk.
Bottom Line: Increased value at less cost will require innovative solutions from those that partner with healthcare providers.
8. The Outpatient Model Pressures the Classic Health System
Everyone is lining up for outpatient care…
- Innovation and improvements in clinical procedures mean that medical or diagnostic procedures that once required an inpatient stay can now be performed safely in an outpatient setting—lowering the risk of contracting a hospital-acquired condition (HAC).
- There has been increasing buy-in from the Center for Medicare and Medicaid Services (CMS); between 2012 and 2019 there were 216 additional reimbursement codes added for outpatient surgeries.
- Medical insurance companies (payers) are attracted by the cost benefits that comes with this shift because inpatient hospitals have costlier services, equipment, and staffing price tags.
- Even patients prefer the convenience of outpatient care. In the 2019 Definitive Healthcare Outpatient Trends Survey, home recovery was reported as the second most important advantage (after cost).
…However, this shift is also introducing new concerns
- As patients dart in and out of clinics, it can be harder to track network leakage and maintain up-to-date, accurate patient records.
- Organizations are realizing that ASCs need constant utilization in order to achieve profitability. so many are turning instead to new marketing strategies in order to attract patients.
- Staffing is a challenge; healthcare organizations are struggling to attract the talent necessary to expand their ambulatory care network.
Learn more
To learn about these eight trends in greater depth, please click here: Healthcare Trends 2020 Webinar Infographic




