Medical claims are some of the most valuable sources of data for healthcare organizations. All-payor claims contain detailed diagnosis and procedure information for any billable patient visit. Healthcare organizations can use this claims information to:
It can be difficult to do all this without fully understanding medical claims data. In this blog, we’ll help you learn the basics about medical claims: what they are, where they come from and what they mean.
What are medical claims?
A medical claim is a bill that healthcare providers submit to a patient’s insurance provider. This bill contains unique medical codes detailing the care administered during a patient visit. The medical codes describe any service that a provider used to render care, including:
- A diagnosis
- A procedure
- Medical supplies
- Medical devices
- Pharmaceuticals
- Medical transportation
How medical claims are generated
When a provider submits a claim, they include all relevant medical codes and the charges for that visit. Insurance providers, or payors, assess the medical codes to determine how they will reimburse a provider for their services. In a value-based care model, length of stay and 30-day readmissions can impact provider reimbursements.
Medical claims vs. pharmacy claims
Medical claims and pharmacy claims capture different aspects of healthcare delivery. Medical claims record services provided by clinicians, hospitals, or other healthcare facilities, such as office visits, procedures, or surgeries. Pharmacy claims, on the other hand, track prescription medications dispensed by pharmacies, including drug type, dosage, and fill dates. While medical claims reflect care delivered, pharmacy claims reflect drug utilization, and together they provide a more complete picture of treatment and costs.
What information medical claims contain
Every medical claims file contains details specific to each patient and patient encounter. In a medical claims file, this information is split in two parts: the claim header and the claim detail.
Claim header
The claim header summarizes the most essential information in the claim. This includes confidential patient information like date of birth, gender, and zip code. The claim header also contains details like:
- National Provider Identifier (NPI) for the attending physician and the service facility
- Primary diagnosis code
- Inpatient procedure, if applicable
- Diagnosis-related group (DRG)
- Name of the patient’s insurance company
- Overall charge for the claim
Claim detail
The claim detail includes information about secondary diagnoses or procedures administered during an inpatient hospital stay. Each new claim detail, or service record, contains the following information:
- Date of service
- Procedure code
- Corresponding diagnosis code
- National Drug Code (NDC), if applicable
- Attending physician’s NPI number
- Charge for the service
What is a medical claims clearinghouse?
A medical claims clearinghouse is an electronic intermediary between healthcare providers and payors. Healthcare providers transmit their medical claims to a clearinghouse. Clearinghouses then scrub, standardize, and screen medical claims before sending them to the payor.
This process helps mitigate errors in medical coding and reduces the time to receive provider reimbursement. If a claim contains medical coding errors or fails to meet formatting requirements, the payor could reject it. This means that the claim would be resubmitted, delaying provider reimbursement.
The service that clearinghouses provide is also beneficial for payors. Clearinghouses format medical claims data according to the unique requirements of each payer. Standardizing the data in this way helps payors streamline their medical billing process.
What is the medical billing process?
The medical billing process involves seven essential steps. These steps trace the entire claims journey from the moment a patient checks in at a healthcare facility, to the moment they receive a bill from their insurance provider.
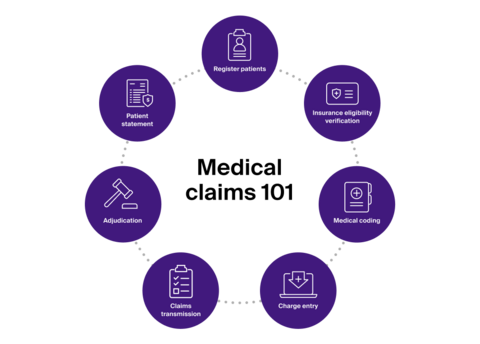
Fig. 1 Illustration of the medical billing process. Circle diagram displays the seven-step process that a medical claim goes through. Illustration from The Definitive Approach to Healthcare Sales – 101: Codifying the Patient Journey.
Patient registration
Patient registration is the very first step in the medical billing process. Registration occurs when a patient gives their provider personal details and insurance information.
Insurance eligibility verification
After a patient has registered, the care provider must verify the patient’s insurance. This helps to confirm that the patient has adequate coverage for the care that they will receive. Verification helps care providers determine coverage and eligibility, and assess the following:
- What the patient’s policy benefits are
- Whether the patient has accumulated co-pay, deductible or out-of-pocket expenses
- Whether the patient’s insurance provider requires pre-authorization
Medical coding
Medical coding is a critical step that occurs after care has been administered. Care providers transcribe their notes and other clinical documentation into standardized medical codes. Some of the most common medical coding systems include:
- Diagnosis-related group (DRG)
- Current procedural terminology (CPT)
- Healthcare common procedure coding system (HCPCS)
- International classification of diseases (ICD-10)
- National drug code (NDC)
Care providers use these codes to describe which medical diagnoses, procedures, prescriptions and supplies they administered and why. The specificity of medical codes also helps providers describe the patient’s condition.
Charge entry
Charge entry is the last step before care providers submit their claim for payment. Providers or medical billing specialists list the charges that they expect to receive.
Claims transmission
Claims transmission is when claims are transferred from the care provider to the payor. In most cases, claims are first transmitted to a clearinghouse. The clearinghouse reviews and reformats medical claims before sending them to the payor.
In some cases, healthcare providers send medical claims directly to a payor. High-volume payors like Medicare or Medicaid may receive bills directly from providers. This helps to reduce the time that it takes to receive reimbursement.
Adjudication
Adjudication occurs once the payor has received a medical claim. The payor evaluates the claim, then decides whether the medical claim is valid and how much of the claim they will reimburse.
If the claim is accepted, the payor will issue provider reimbursement and charge the patient for any remaining amount. The payor may deny the claim if the patient has insufficient coverage or did not get pre-authorization for a service. If a payor denies a medical claim, the patient may have to submit an appeal to gain coverage for the care costs.
The payor may also reject a claim. This happens when the claim does not meet formatting requirements or contains an error in medical coding. Rejected medical claims can be resubmitted for payment once the errors have been corrected.
Patient statement
Patient statement is the final step in the medical billing process. Once the payor has reviewed a medical claim and agreed to pay a certain amount, they bill the patient for any remaining costs.
How medical claims data is used in healthcare
De-identified medical claims data helps organizations understand patterns of care and identify opportunities in the healthcare market. Real-world use cases include:
- Pharma and medical device companies: Size markets, identify high-value providers, prioritize accounts, plan product launches, and guide go-to-market and contracting strategies.
- Healthcare providers and health systems: Improve operations, allocate staff and resources, close gaps in care, expand service lines, streamline patient pathways, and improve patient outcomes.
- Consulting, technology, and service companies: Pinpoint where solutions can have the most impact, identify growth or efficiency opportunities, and align services with provider needs.
- Medical suppliers, staffing firms, and other industries: Track utilization trends, prioritize territories and accounts, and ensure the right products and professionals reach the right facilities.
Limitations and considerations of medical claims data
While medical claims data is a powerful tool for understanding care patterns and guiding business decisions, it has important limitations. Claims reflect billed services, not clinical outcomes, so they may not capture the full patient experience. Data can lag, sometimes by several months, due to the claims submission and adjudication process.
Additionally, claims data often lacks context for non-billable activities, such as patient education. To make more informed decisions, organizations should use claims data alongside other sources like market intelligence, medical and scientific expert data, or consumer analytics.
Learn more
Manually acquiring, cleansing, and analyzing medical claims data is a laborious and time-consuming process—and once you’ve built your dataset, you’ll need to routinely update and maintain it. If you want instant, hands-on access to the latest medical claims data, provider profiles, and powerful analytics, our healthcare data platform puts everything you’re looking for in one place.
Schedule a free trial today and we’ll show you how to use claims data to target sales opportunities, understand buyers, and grow your business.




